Cancer 101
Join for free on the MyCancerHaven platform to learn even more about Amyloidosis with access to more educational videos, expert opinions, blogs, news, information, channels for communication and much more.
What is AL Amyloidosis?
AL Amyloidosis, also known as primary amyloidosis, is a rare disorder characterized by the abnormal accumulation of a protein called amyloid in various organs of the body. This protein buildup can interfere with the normal function of these organs. AL Amyloidosis is considered the most common type of amyloidosis.
Understanding 'AL' in AL Amyloidosis: The 'AL' in AL Amyloidosis stands for 'Amyloid Light-chain.' This refers to the specific type of protein that is overproduced and leads to the disease. These light-chain proteins are components of antibodies created by your bone marrow. In AL Amyloidosis, the bone marrow generates an excessive amount of these proteins. When these proteins cannot be properly broken down, they begin to accumulate in different parts of the body, forming what is known as amyloid deposits.
Where does AL Amyloidosis affect?: These amyloid deposits can form in any organ within the body, including the heart, kidneys, liver, and nerves. The specific symptoms that an individual experiences will largely depend on the organs affected by these deposits.
Causes and Prevention of AL Amyloidosis: The exact reason why certain individual's plasma cells start to behave abnormally, leading to AL Amyloidosis, is not entirely understood. Importantly, it is not a contagious condition and is not thought to be caused by lifestyle factors such as diet or exercise. As of now, there are no known preventive measures for AL Amyloidosis, as most instances of the disease appear to occur randomly.
Is AL Amyloidosis hereditary?: While a family history can increase the risk for some types of amyloidosis, AL Amyloidosis is not typically considered a hereditary condition. It is not passed down from parents to their children through genes.
Incidence and Prevalence of AL Amyloidosis: The incidence of AL Amyloidosis, referring to how often new cases occur, is estimated to be between 1 and 3 new cases per 100,000 people annually in the United States. It can affect adults of any age, but is most commonly diagnosed in individuals between the ages of 60 and 70. The prevalence, or how many people have the disease at any given time, is more challenging to estimate due to the rarity of the disease and the wide variety of symptoms it can cause. Some individuals might live with the disease for an extended period without realizing it, as their symptoms may be mild or mistaken for other conditions.
What are the symptoms of AL Amyloidosis?

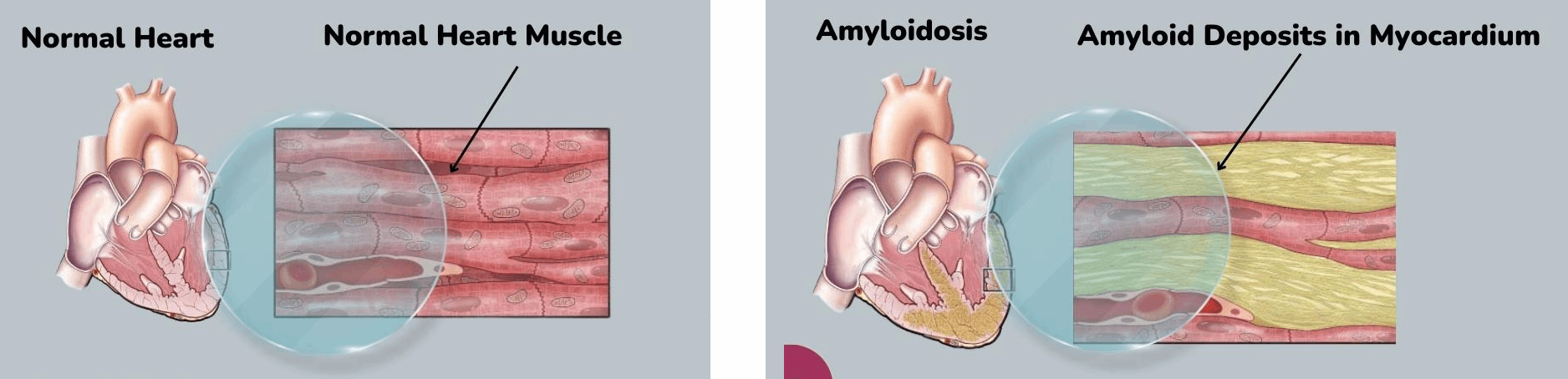
1. Symptoms related to the heart (Cardiac Amyloidosis): In cases where amyloid proteins accumulate in the heart, it can result in cardiac amyloidosis. The heart may struggle to function properly, causing individuals to experience fatigue or shortness of breath. Irregular heartbeats and swelling in the legs and ankles might also be observed.
2. Symptoms related to the kidneys (Renal Amyloidosis): When the kidneys are affected by the build-up of amyloid proteins, their ability to filter blood can be compromised. This can lead to protein leakage into the urine, causing swelling in the legs and ankles. Over time, this might progress to kidney failure, manifesting as symptoms such as fatigue, nausea, loss of appetite, or general weakness.
3. Symptoms related to the nervous system: If amyloid proteins impact the nerves, individuals may experience numbness, tingling, or pain in their fingers and toes, a condition known as peripheral neuropathy. If the autonomic nerves controlling blood pressure are affected, one might experience lightheadedness or even fainting upon standing.
4. Symptoms related to the gastrointestinal tract: If the digestive system is affected, individuals may experience a loss of appetite, weight loss, diarrhea, or constipation.
5. Symptoms related to the liver: Amyloidosis in the liver may cause the organ to enlarge, leading to a feeling of fullness or discomfort in the upper abdomen.
6. Symptoms related to soft tissues: Amyloid deposits can lead to conditions like carpal tunnel syndrome or an enlarged tongue, which can cause difficulty swallowing or breathing.
7. Symptoms related to the skin: Individuals may notice changes in their skin, such as easy bruising or purplish patches around the eyes.
It's important to note that these symptoms can be associated with many other conditions as well, so their presence does not definitively indicate AL amyloidosis. However, persistent or worsening symptoms should prompt a medical consultation. A doctor can perform tests to ascertain the cause of the symptoms and develop an appropriate treatment plan.
How is AL Amyloidosis diagnosed?

Diagnosing AL amyloidosis can be a bit complex because its symptoms can be similar to those of other diseases. The general process involves:
1. Medical History and Physical Examination: A doctor will start by asking patients about their symptoms, overall health, and any previous medical conditions and conduct a physical examination.
2. Blood and Urine Tests: These tests help identify abnormal proteins in the blood or urine. They can suggest the presence of amyloidosis, but they can't confirm the diagnosis on their own.
3. Biopsy: A biopsy is a procedure where a small sample of tissue is removed from the body and examined under a microscope. For amyloidosis, the biopsy could be taken from various places, such as fat tissue, bone marrow, or an organ like the kidney heart or liver. The biopsy can show whether amyloid proteins are present and also help determine the type of amyloidosis.
4. Imaging Tests: Doctors might use imaging tests like echocardiograms (an ultrasound for the heart), CT scans, or MRI scans. These tests can show whether organs, like the heart or kidneys, are enlarged or have any other changes that might be due to amyloidosis.
5. Genetic Testing: In some cases, genetic tests may be used to identify hereditary forms of amyloidosis. This test would not be typically used for diagnosing AL amyloidosis as it is not a hereditary condition, but it might be used to rule out other types.
6. Serum Free Light Chain Assay and Ratio: This is a specific blood test that can help confirm the diagnosis of AL amyloidosis. It measures the levels of light chains, the specific type of protein that causes AL amyloidosis, in the blood.
It's important to remember that this diagnosis process can take time. If a patient is worried about their symptoms or if they have been diagnosed with AL amyloidosis, it's important to talk to the healthcare team. They can provide more specific information based on each unique situation.
How is AL Amyloidosis treated?

The treatment for AL amyloidosis primarily focuses on reducing the production of the abnormal light chain proteins that form amyloid deposits, and managing the symptoms related to organ involvement. The specific plan often depends on how far the disease has progressed and which organs are involved. Some typical treatments include:
1. Chemotherapy and Steroids: In AL amyloidosis, the amyloid proteins are made by cells in the bone marrow. Certain chemotherapy drugs can help control the growth of these cells, which reduces the amount of abnormal protein they produce. Steroids can also be used to slow down the production of these proteins.
2. Targeted Therapy: Some newer treatments specifically target the abnormal cells in the bone marrow. These include drugs like bortezomib, lenalidomide, or daratumumab, which have been used in the treatment of other bone marrow diseases like multiple myeloma, and have shown promise in treating AL amyloidosis.
3. Autologous Stem Cell Transplant (ASCT): Some patients may be eligible for this procedure, which involves high-dose chemotherapy to kill the cells in the bone marrow that are producing the abnormal proteins, and then replenishing the bone marrow with the patient's own healthy stem cells. This is a complex procedure with potential risks and benefits that need to be carefully evaluated.
4. Supportive Care: This focuses on managing the symptoms and improving the quality of life. For example, diuretics can help manage fluid retention caused by heart or kidney involvement, and special diets may be recommended if the disease is affecting the digestive system.
5. Clinical Trials: Because AL amyloidosis is a rare condition, new treatments are being researched in clinical trials. Participating in a clinical trial can provide access to promising new treatments that aren't yet widely available.
Every patient's situation is unique, so treatment plans can vary. It's important to have in-depth discussions with one’s healthcare team about the most suitable treatment plan. They can explain the potential benefits, risks, and side effects of each treatment, and help patients make the best decision based on their condition and lifestyle.













